Indicate Whether Each Item Identifies An Adaptive Or Innate Immunity
Onlines
Apr 04, 2025 · 7 min read
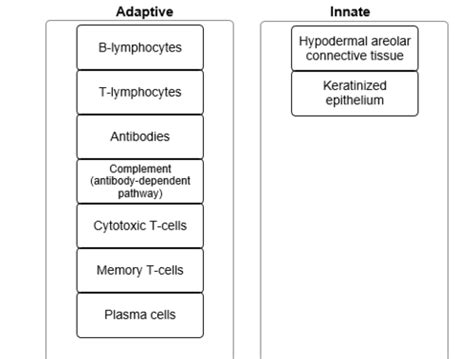
Table of Contents
Adaptive vs. Innate Immunity: A Comprehensive Guide
The human immune system is a complex network of cells, tissues, and organs working tirelessly to defend against a constant barrage of pathogens. This defense is broadly categorized into two arms: innate immunity and adaptive immunity. Understanding the distinction between these two systems is crucial for comprehending how our bodies fight off infections and maintain health. This article will delve deep into the characteristics of each, providing detailed examples to clarify the differences.
Innate Immunity: The Body's First Line of Defense
Innate immunity, also known as non-specific immunity, is the body's immediate, non-specific response to infection. It's the first line of defense, acting rapidly to prevent pathogens from establishing themselves. Unlike adaptive immunity, innate immunity doesn't improve with repeated exposure to the same pathogen. Its key characteristics include:
- Non-specific: It attacks any foreign invader, regardless of its identity.
- Rapid response: It acts within minutes to hours of encountering a pathogen.
- No immunological memory: It does not retain memory of past infections, meaning the response remains the same upon subsequent encounters with the same pathogen.
Let's examine the key components of innate immunity:
1. Physical Barriers: The Body's Initial Shield
The first level of innate immunity involves physical barriers that prevent pathogen entry. These include:
- Skin: The skin's outer layer, the epidermis, forms a tough, waterproof barrier. Its slightly acidic pH inhibits bacterial growth. The shedding of skin cells also helps remove pathogens.
- Mucous Membranes: These line the respiratory, gastrointestinal, and genitourinary tracts. Mucus traps pathogens, and cilia (tiny hair-like structures) sweep them away.
- Tears and Saliva: These contain lysozyme, an enzyme that breaks down bacterial cell walls.
2. Chemical Barriers: A Chemical Assault on Pathogens
Chemical barriers complement the physical barriers, actively inhibiting pathogen growth:
- Stomach acid: The highly acidic environment of the stomach kills most ingested pathogens.
- Sebum: An oily secretion from sebaceous glands in the skin, sebum inhibits bacterial growth.
- Antimicrobial peptides: These small proteins directly kill microbes or inhibit their growth. Examples include defensins and cathelicidins.
3. Cellular Components: The Innate Immune Cells
If pathogens breach the physical and chemical barriers, innate immune cells are mobilized to combat the threat. These include:
- Phagocytes: These cells engulf and destroy pathogens through a process called phagocytosis. Key phagocytes include:
- Neutrophils: The most abundant type of white blood cell, neutrophils are the first responders to infection, rapidly migrating to the site of inflammation.
- Macrophages: These are large phagocytes that reside in tissues, acting as sentinels and engulfing pathogens and cellular debris. They also play a vital role in initiating the adaptive immune response.
- Dendritic cells: These antigen-presenting cells capture antigens from pathogens and present them to T cells, initiating the adaptive immune response.
- Natural Killer (NK) Cells: These lymphocytes recognize and kill infected or cancerous cells without prior sensitization. They release cytotoxic granules containing perforin and granzymes, which induce apoptosis (programmed cell death) in target cells.
- Mast Cells and Basophils: These cells release histamine and other inflammatory mediators, contributing to the inflammatory response.
4. Inflammatory Response: A Localized Battle
Inflammation is a critical component of innate immunity. It's a complex process characterized by:
- Redness: Increased blood flow to the infected area.
- Swelling: Accumulation of fluid in the tissues.
- Heat: Increased temperature due to increased blood flow.
- Pain: Activation of pain receptors due to tissue damage and inflammatory mediators.
- Loss of function: Impaired function of the affected area.
Inflammation helps to contain the infection, recruit immune cells to the site of infection, and promote tissue repair.
5. Complement System: A Cascade of Defense
The complement system is a group of proteins circulating in the blood that enhance the ability of antibodies and phagocytes to clear microbes and damaged cells. Activation of the complement system leads to:
- Opsonization: Coating pathogens to make them more susceptible to phagocytosis.
- Chemotaxis: Attracting phagocytes to the site of infection.
- Formation of membrane attack complexes (MACs): These complexes create pores in the pathogen's membrane, leading to its lysis (destruction).
Adaptive Immunity: A Targeted and Precise Response
Adaptive immunity, also known as acquired immunity, is a more specific and targeted response to infection. It's slower to develop than innate immunity but offers long-lasting protection against specific pathogens. Key characteristics include:
- Specificity: It targets specific pathogens or antigens.
- Memory: It retains memory of past infections, leading to a faster and stronger response upon subsequent encounters with the same pathogen.
- Self-tolerance: It can distinguish between self and non-self antigens, preventing attacks on the body's own tissues.
The two main arms of adaptive immunity are:
1. Humoral Immunity: Antibody-Mediated Defense
Humoral immunity is mediated by B cells, which produce antibodies. Antibodies are proteins that bind to specific antigens (foreign substances) on the surface of pathogens. This binding can lead to:
- Neutralization: Blocking the pathogen from infecting cells.
- Opsonization: Enhancing phagocytosis.
- Activation of the complement system: Leading to pathogen lysis.
2. Cell-Mediated Immunity: A Cellular Assault
Cell-mediated immunity is mediated by T cells. There are several types of T cells:
- Helper T cells (CD4+ T cells): These cells release cytokines, signaling molecules that activate other immune cells, including B cells and cytotoxic T cells.
- Cytotoxic T cells (CD8+ T cells): These cells directly kill infected or cancerous cells by releasing cytotoxic granules containing perforin and granzymes.
- Regulatory T cells (Treg cells): These cells suppress the immune response, preventing autoimmune reactions.
Antigen Presentation: Bridging Innate and Adaptive Immunity
A crucial link between innate and adaptive immunity is antigen presentation. Antigen-presenting cells (APCs), such as dendritic cells and macrophages, engulf pathogens, process their antigens, and present them on their surface bound to major histocompatibility complex (MHC) molecules. These MHC-antigen complexes are recognized by T cells, initiating the adaptive immune response.
Comparing Innate and Adaptive Immunity: A Table Summary
| Feature | Innate Immunity | Adaptive Immunity |
|---|---|---|
| Specificity | Non-specific | Specific |
| Response Time | Rapid (minutes to hours) | Slow (days to weeks) |
| Memory | No immunological memory | Immunological memory (long-lasting protection) |
| Components | Physical barriers, chemical barriers, phagocytes, NK cells, complement system, inflammation | B cells, T cells, antibodies |
| Mechanism | Direct attack, inflammation, complement activation | Antibody production, cell-mediated cytotoxicity |
Examples Differentiating Innate and Adaptive Immunity
To further clarify the distinctions, let's examine some specific examples:
Innate Immunity Examples:
- A cut on your finger: The skin barrier is broken, but the innate immune system responds immediately with inflammation, recruiting neutrophils and macrophages to fight off any invading bacteria.
- A viral infection: NK cells recognize and kill virus-infected cells before the adaptive immune response is fully engaged.
- The inflammatory response to a splinter: Redness, swelling, heat, and pain are all hallmarks of the innate immune system's response to injury and infection.
Adaptive Immunity Examples:
- Chickenpox: After recovering from chickenpox, you develop immunity to the varicella-zoster virus due to the generation of immunological memory by B and T cells.
- Measles vaccination: The vaccine introduces a weakened form of the measles virus, triggering an adaptive immune response, leading to the production of antibodies and long-lasting immunity.
- Tuberculosis infection: The adaptive immune response, specifically cell-mediated immunity, is crucial for controlling the infection caused by Mycobacterium tuberculosis.
Conclusion: A Collaborative Defense System
Innate and adaptive immunity work together in a coordinated fashion to protect the body from infection. Innate immunity provides the initial, rapid response, while adaptive immunity provides a more targeted and long-lasting defense. This intricate interplay between the two systems is essential for maintaining health and preventing disease. Understanding this complex relationship allows for a greater appreciation of the body's remarkable ability to defend itself against a vast array of pathogens. Further research continues to unveil the intricacies of this fascinating and vital biological process.
Latest Posts
Latest Posts
-
When Workers Are Asked To Participate In A Research Study
Apr 04, 2025
-
American Red Cross Exam A Answers
Apr 04, 2025
-
The Case Of The Desert Bones Analysis Questions
Apr 04, 2025
-
The Chaser By John Collier Summary
Apr 04, 2025
-
Veterans Have Expressed That Its Important To Get Appointments
Apr 04, 2025
Related Post
Thank you for visiting our website which covers about Indicate Whether Each Item Identifies An Adaptive Or Innate Immunity . We hope the information provided has been useful to you. Feel free to contact us if you have any questions or need further assistance. See you next time and don't miss to bookmark.
